Corneal Cross-Linking
Also known as CXL
Medical Disclaimer: Information on this page is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
See our Terms for details.

Overview
Corneal cross-linking (CXL) is a minimally-invasive, in-office procedure that strengthens a weak or bulging cornea by creating new chemical bonds between collagen fibers. A combination of vitamin B2 (riboflavin) eye drops and controlled ultraviolet-A (UVA) light stiffens the cornea, halting — and often flattening — progressive disorders such as keratoconus and post-LASIK ectasia. Approved by the U.S. FDA in 2016, CXL is now performed worldwide and has reduced the need for corneal transplants in young adults with keratoconus.12
How the Procedure Works & Options
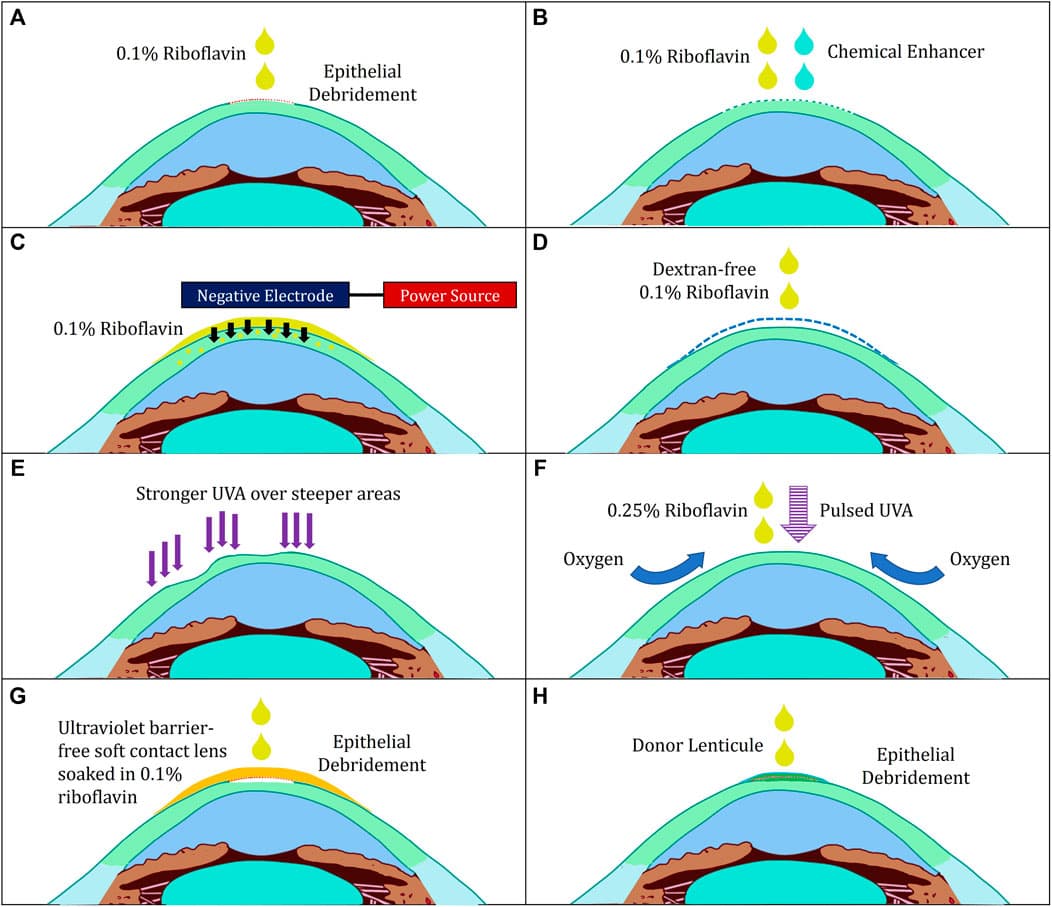
CXL relies on photochemical hardening. Riboflavin saturates the corneal stroma and, when exposed to UVA (365 nm), generates reactive oxygen species that form new covalent bonds between collagen fibrils. The FDA-approved epi-off Dresden protocol removes the thin surface epithelium, applies 0.1 % riboflavin for 30 minutes, then shines 3 mW/cm2 UVA for another 30 minutes. Alternatives include accelerated protocols (9 mW/cm2 for 10 minutes) and epi-on protocols that leave epithelium intact, trading comfort for slightly less biomechanical stiffening. Custom or patterned CXL is being studied to flatten only the cone apex while sparing peripheral vision.34
Who Is a Candidate?
The best candidates are people 12–45 years old with documented progression of keratoconus or post-refractive-surgery ectasia. Warning signs include: steepening ≥1.0 D on topography, Kmax ≥47 D, thinning to <500 µm, or worsening glasses prescription. CXL can also stabilize pellucid marginal degeneration and some corneal infections under compassionate-use protocols. It is not recommended in corneas thinner than 375 µm after epithelial removal, active herpetic keratitis, severe dry eye, or pregnancy. Studies show earlier treatment preserves two or more lines of best-corrected vision versus delayed treatment.56
Benefits and Limitations
Benefits
• Stops or slows cone progression in 85–90 % of eyes.
• About 40 % gain one or more lines of vision as the cone flattens.
• One-time treatment with long-term biomechanical stability.
Limitations
• Vision may blur for several weeks while the surface heals.
• Cannot reverse scarring or deep corneal opacities; transplant may still be needed in advanced cases.
• Insurance coverage varies and may require progression documentation.
The AAO Ophthalmic Technology Assessment found epi-off CXL more effective than rigid lenses or observation in preventing keratoconus progression over 3 years.78
Risks and Side Effects
Most people experience scratchy pain, light sensitivity, and tearing for 3–5 days until the epithelium regrows. Serious complications are uncommon but include infectious keratitis (≈1 %), corneal haze or scarring (up to 10 %, usually transient), sterile infiltrates, and delayed epithelial healing. Rare endothelial damage may occur if the cornea is too thin. Proper riboflavin soaking, intra-operative pachymetry, and UV power calibration keep complication rates low.910
Recovery and Long-Term Care
After surgery, a bandage contact lens and antibiotic/steroid drops are used for one week. Vision usually returns to pre-op levels within 1–3 months, then gradually improves. Follow-up visits at 1 day, 1 week, 1 month, 3 months, 6 months, and 1 year monitor epithelial healing and Kmax. Rigid or scleral lenses are refit after the 6-week mark once the cornea stabilizes. UV-blocking sunglasses are essential for the first 30 days to protect the photosensitized cornea.11
Latest Research & Innovations
Accelerated CXL using higher irradiance (9–30 mW/cm2) shortens UVA exposure to 3–10 minutes, with comparable stiffening when pulsed illumination is used. Epi-on protocols add enhancers (benzalkonium chloride, EDTA, or iontophoresis) to drive riboflavin through intact epithelium for faster, more comfortable recovery. Trials are exploring photoactivated chromophore for infectious keratitis (PACK-CXL) to treat resistant corneal ulcers, and intrastromal ring + CXL combinations to improve vision in advanced cones. Gene therapy targeting collagen cross-linking enzymes and femtosecond-laser-assisted patterned CXL are on the horizon.1314
Next Steps – See a Cornea Specialist
If your glasses prescription or corneal map is changing, a consultation with a cornea specialist can determine whether CXL can preserve your vision. The doctor will review topography, pachymetry, and visual acuity trends, then explain timing, costs, and expected outcomes. You can connect with the right expert on Kerbside and take proactive steps to protect your cornea today.
Bring prior eye scans, a list of contact-lens parameters, and note any allergy to riboflavin or anesthetics so the visit is efficient and personalized.1516